Frequently Asked Questions – Cataract
What is a cataract?
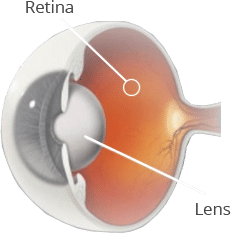
A cataract is a condition where the natural lens of our eye starts to turn cloudy or opaque. This is usually caused by the accumulation of protein as we progress in age. Cataracts result in a blurred and/or decreased field of vision. We may also perceive a drop in contrast and colour perception in the early stages of the condition.
What are the different types of cataracts?
There are 3 main types of cataracts:
1 Nuclear
The most common type of cataract, the clouding occurs in the nucleus or the centre of the lens.
2 Posterior sub-capsular
Posterior sub-capsular – This forms at the back of the lens as an opaque area. It arises in individuals who are diabetic and who are on prolonged use of steroids.
3 Cortical
Cortical – Occurring on the cortex or the periphery of the lens, the clouding works its way towards the centre like spokes in a wheel.

What causes cataracts?
By and large, cataracts are a natural result of ageing. However, there may be other contributing factors:
- Congenital (a family history of cataract)
- Obesity
- Poorly managed diabetes
- Smoking
- Drinking alcohol
- Eye trauma
- Inflammation
- Having previously undergone eye surgery such as refractive surgery
- A high degree of short-sightedness (myopia)
- Exposure to ultra-violet radiation from the sun
- Exposure to ionising radiation from X-rays and gamma rays
- Prolonged use of medication that contain steroids such as steroid eyedrops, oral steroids, nasal steroid sprays, etc
Are cataracts inevitable?
They are almost inevitable as we age, hence individuals over the age of 40 should have their eyes checked regularly as a precaution.
Can younger people get cataracts?
Cataracts in young people are not as common. If they are present, it could be due to one or more of the contributing factors stated previously here.
What are the symptoms of cataracts?
During the initial stages, the effects of cataracts are hard to make out as the changes to vision are marginal. As the condition evolves, you may find it increasingly difficult to carry out daily tasks such as reading and driving. When this happens, consult with an eye specialist immediately.
The symptoms of cataracts include:
- Cloudy or blurred vision
- Haziness in the form of a ‘film’ over the eye
- Extreme glare from sunlight, lamps, or car headlights
- Haloes around bright lights
- Hard to see in dim light or at night
- Encountering a brown or yellow tinge in your vision
- Faded or less saturated colours
- A case of double vision
- Frequently changing prescriptions for spectacles or contact lenses
Cataracts usually do not cause any pain, discomfort or redness in the eye. However, there may be symptoms of pain and nausea if they are associated with increased intraocular pressure (the build-up of fluid pressure within the eye).
How to prevent cataracts from getting worse?
As cataracts develop gradually, it may take several years before individuals find it difficult to complete their daily tasks. The progression unfortunately is not reversible. However, you can take some measure to help slow them down:
- Make appointments to see your eye doctor regularly as early discovery allows you to manage your condition better.
- Keep to a balanced diet of leafy vegetables, fish rich in omega-3 fatty acids, citrus fruits, whole grains and nuts.
- Protect your eyes from the sun by wearing caps with long visors or wide-brimmed hats and/or sunglasses with adequate UV protection.
- Keep your eye doctor informed of the prescription medication that you are on, for example, steroids, as they may have the side effect of quickening cataract development.
- Keep your diabetes under control.
- Quit smoking and reduce your intake of alcohol.
Can cataracts be treated with eyedrops?
There are currently no FDA-approved eyedrops that can treat cataracts. There is research being conducted however that involves a naturally occurring steroid called lanosterol that can be administered via eyedrops but the findings have been inconclusive so far.
When to check for cataracts?
It is advisable to go for regular eye check-ups once you turn 40 to check not only for cataracts, but for other conditions that may affect your vision such as refractive errors, retinal tears, floaters, glaucoma, and macular degeneration.
Under certain circumstances, it is possible to have these other conditions corrected at the same time as your cataract surgery, for example if you have both glaucoma and cataracts. When your cataracts are being removed, surgery can also be performed to decrease intraocular pressure within the eye and hence decrease the need for glaucoma eyedrops.
How do doctors check for cataracts?
A number of tests will be conducted to determine if you have cataracts:
Firstly, your eye prescription will be checked. This process is called Manifest Refraction and it involves the placing of lenses of varying degrees in front of your eyes.
Next, your intraocular pressure (IOP) will be tested via a puff of air on your cornea. An instrument measures the momentary flattening of your cornea to give your IOP reading. This gives an indication of whether you are at risk of glaucoma.
Finally, the doctor will examine your eye to confirm the presence of cataracts. Eyedrops will be administered first to dilate the pupil of your eye. After 30 minutes, your pupil will be sufficiently dilated for the doctor to use a Slit Lamp to check for signs of cataracts as well as for other conditions in your eye. If there are cataracts, a photograph will be taken to evaluate the condition further and also to serve as a record of the condition pre-surgery.
After all the tests are completed, you will consult with the doctor to discuss the findings and explore the options that are available to you.
What is the history of cataract surgery?
Modern cataract surgery came about from the development of intraocular lens implantation in 1949 and phacoemulsification in 1967. The latter is a method utilising ultrasonic vibrations to break up cataracts into small particles, which are then removed using a small probe. Ever since then, cataract surgery has been the only way to effectively treat cataracts.
What are the main types of cataract surgery?
There are 2 main ways of cataract removal during surgery:
Micro-incision phacoemulsification surgery – the cataracts in the lens of the eye are liquified by ultrasound energy. The emulsified remnants are then removed via a narrow incision measuring 2 to 3mm. As the wounds are self-healing, no stitches (sutures) are required, allowing for a faster recovery.
Laser-assisted cataract surgery (also known as FLACS; femtosecond laser-assisted cataract surgery) – this procedure utilises the femtosecond laser used in LASIK surgery to create the incision and fragment the cataract. Ideal for complex surgeries, this method is also seen as being minimally invasive, has improved wound construction, and allows for accurate lens positioning. However, the procedure costs more than micro-incision phacoemulsification surgery and its benefits are not seen as significant enough to warrant the price differential.
Am I suitable for phacoemulsification cataract surgery?
Most people with cataracts are suitable for micro-incision phacoemulsification surgery. Your surgeon will look at all possible factors to assess your suitability including your age, health, and medical prescriptions. There are several conditions that come with increased risks, such as diabetes (see here for more details), macular degeneration and a detached retina.
Am I suitable for laser-assisted cataract surgery?
Current studies have shown that patients with moderately advanced cataracts, large pupils and clear corneas are suitable for FLACS (femtosecond laser-assisted cataract surgery). Patients who have undergone radial keratotomy or have opaque corneas may not be suitable candidates for FLACS as the corneal scars or opacities affect the transmission of the laser across the cornea to the lens.
Am I suitable for cataract surgery if I have diabetes or other systemic condition?
There are cataract patients who may also suffer from diabetes and other systemic conditions (diseases that affect other parts of the body). For such patients, cataract surgery may place additional stress on the eye and this can lead to macular edema, progressive retinopathy, and/or limited vision.
It is still possible to have successful cataract surgery in patients with diabetes, however, there is an increased risk of complications and affected vision. If extra care is taken during the pre-operative stage, during phacoemulsification, and there is close supervision post-surgery, diabetic patients can expect optimal outcomes.
What are the replacement lens options for cataract surgery?
After the removal of cataracts (the natural lens), an artificial intraocular lens (IOL) will be inserted via a small incision of between 2 and 3mm and positioned correctly. The lens is left there permanently and need not be replaced.
Generally speaking, there are 3 types of IOLs:
- Monofocal IOL – it corrects a specific part of your visual range, usually for near, mid or far vision. Due to only one focus being selected (most individuals will opt for far vision), spectacles will still be required.
- Multifocal IOL – similar to progressive spectacles, these lenses have different zones which allow for focusing on objects that are near or far. Multifocal IOLs can also be used to correct presbyopia.
- Extended Depth of Focus (EDOF) – this IOL aim to provide 2 zones of vision (intermediate and far) which will enable patients to view their computer screens and drive without the use of glasses. Reading glasses are still required for near tasks. However, as it does not have the ‘rings’ optics found in multifocal IOLs, patients are less likely to see halos and glare.
In addition to the above IOLs, there are also Toric IOLs which can help correct astigmatism, the condition where the cornea or lens is irregularly shaped. Toric IOLs have different powers in different meridians of the lens, which when properly aligned, are able to correction astigmatism.
Although rare, and depending on how the eye heals, an individual may still have remaining refractive errors after the implantation of an IOL. In these cases, the error may be corrected by laser vision correction such as LASIK or the patient has to continue wearing glasses.
When is the best time for cataract surgery?
In the past when the technology was not advanced, the eye lens could only be extracted safely when the cataract was ‘ripe’ or ‘mature’, that is, when it was in an advanced state.
Today, this is no longer a concern as it can be removed at any stage of development. In fact, waiting too long to get surgery done may increase the risk and complexity of the procedure.
So, when is it recommended to have the surgery? The answer is when cataracts are impairing your vision to a degree that prevents you from going about your daily activities.
You may delay having surgery if you can still conduct your daily activities with ease, however, as cataracts tend to affect eye prescription, you need to have your vision checked yearly and make new pairs of glasses if necessary.

When is the right age to have cataract surgery?
There is no right age to have the surgery, although as one gets older, there is an increased risk if one has other age-related medical conditions.
However, cataract patients are getting younger and it may not necessarily be due to the age-related risk:
- There is greater awareness (as a result of what is found online) about not waiting until cataracts are mature to get surgery done.
- Improvements in technology which gives one a greater sense of confidence in the procedure.
- Ability to use Medisave and insurance for the surgery.
- The surgery being used as a refractive procedure – many younger patients will opt for Refractive Cataract Surgery to remove their cataracts while at the same time, correct their refractive conditions such as myopia, hyperopia, and astigmatism – read here to find out more.
Contact us today for more information and booking appointments.
Is cataract surgery painful?
The majority of patients do not feel any pain during and after the surgery. Note that anaesthetic (numbing) eyedrops are applied during surgery to maximise your comfort. There are some patients however, who may experience mild discomfort after the surgery when the anaesthetics wear off. This is temporary and can be treated with over-the-counter pain medication. For more information on anaesthesia during cataract surgery, please read here.
What are the side effects of cataract surgery?
There is the possibility of certain side effects occurring after cataract surgery. The most common ones are dry eye and night vision problems. They are usually temporary, lasting about 3 months and tapering off as the days go by. For night vision problems, they are more prominent with multifocal IOLs. For all types of IOL on the other hand, floaters may become more visible due to the clarity gained after the procedure.
It is important to monitor your condition closely after surgery – if you find increased redness and/or blurring of vision, swelling, tearing or sharp pains, please contact your doctor immediately.
Can cataracts return after surgery?
No, they do not return once they are removed.
What are the risks of cataract surgery?
Cataract surgery has low risks. In the case of infections for example, the incidence rate is about 1 in 1,000 people.
The following are some of the rare complications that may arise from surgery:
- Endophthalmitis – an inflammation of the eye. To treat this infection, antibiotics are administered via intravitreal injection. Vision loss may occur if left untreated.
- Posterior capsular rupture – cataract fragments falling into the back of the eye. If this occurs, another procedure will be performed to remove them.
- Posterior capsular opacification – cloudiness that appear months or years after the surgery. As cataracts do not return, this is caused by scar tissue forming behind the lens implant. YAG laser capsulotomy surgery can be performed to correct the problem.
Can cataract surgery be performed on both eyes at the same time?
Some patients may opt for this as a form of convenience. The procedure is called bilateral cataract surgery. The benefits of this are fewer visits to the doctor and a quicker recovery period.
However, many eye doctors recommend separate procedures for each eye. This allows for a proper evaluation of the results from the first eye before proceeding to the next. In addition, although there is a low risk of complications arising, if infection occurs in both eyes, the patient would be ‘out-of-action’ for a period of time.
Do I need glasses/contact lenses after cataract surgery?
This depends on the type of IOL that is implanted during your surgery. If it is a multifocal IOL, you usually do not have to wear glasses after the surgery. If it is a monofocal IOL for long-distance vision, you may still need reading glasses after the surgery.
Likewise, for contact lenses, it will depend on the type of IOL that is implanted during surgery.
If one eye is operated on first, you can wear a contact lens in the unoperated eye for the duration it takes for the first eye to stabilise, that is, several weeks to a month.
Can I have cataract surgery after LASIK?
Cataract surgery is possible if you have undergone LASIK (or ReLEx SMILE). Take note however, that due to the change in the shape of the cornea after LASIK, a more detailed assessment needs to be performed on your eye to calculate the required IOL power.
If you have had LASIK done before, surgeons generally discourage the use of multifocal IOLs as it is challenging to accurately match the lens to the cornea. Monofocal IOLs for distance vision are recommended instead so reading glasses will still be required post-surgery.
Can cataract surgery correct myopia, hyperopia, and astigmatism?
Yes, by selecting an appropriate IOL, you can correct just about any degree of hyperopia, myopia and even astigmatism at the time of surgery. This procedure is called Refractive Cataract Surgery.
Can cataract surgery correct presbyopia?
It is common for many cataract patients to also have presbyopia as both are age-related conditions. You can correct your presbyopia at the same as your cataract surgery by implanting a multifocal IOL.
How do I prepare for cataract surgery?
You are required to fast a minimum of 6 hours before the surgery.
You are advised to arrange for someone to take you home after the surgery or return home on your own via a taxi.
As your eyes may be sensitive to bright lights after the surgery, bring a pair of sunglasses with you.
How long does cataract surgery take?
The cataract procedure is considered a day surgery; you are not required to stay overnight. The duration of your stay in the hospital is about 2 to 3 hours although the procedure itself lasts 30 minutes for 1 eye – read more here about having surgery performed on both eyes on the same day.
What happens during cataract surgery?
Cataract surgery is usually performed under topical anaesthesia (also known as local anaesthesia). This means that you are awake and able to communicate with the surgeon during the surgery.
Anaesthetic eyedrops or an injection will be administered to numb the area around your eye. You may also be given intravenous sedation to help you relax – you will be required to undergo a pre-op ECG and blood test to check if you are suitable for the sedation.
During the surgery, you will hardly feel any pain although some patients may feel a little discomfort.
There are rare instances during surgery where it is discovered that a patient is unsuitable to have a multifocal IOL implanted. In such cases, a monofocal IOL will be implanted instead.
Can one choose general anaesthesia during cataract surgery?
Cataract surgery is commonly performed under topical anaesthesia. There are cases where general anaesthesia (to make the patient unconscious) is more suitable, for example, if the complexity of the surgery is high or if the patient is unable to hold a steady gaze. For individuals who feel anxious about feeling pain or discomfort during surgery, general anaesthesia may be administered but only after passing a pre-anaesthetic evaluation.
How long does it take before I can see after cataract surgery?
It usually takes several hours after the surgery before you can have a semblance of clear vision. You may, however, take as long as a week or two before your focus is at its sharpest.
What is the recovery time for cataract surgery?
Your vision will fluctuate over the following days; on some days it is clearer while on other days it is blurrier. Expect 3 months before your vision fully stabilises.
How many times does one have to come back for review after cataract surgery?
Typically, you are required to return for reviews after the surgery; 1 day, 1 week, 1 month, 6 months and 1 year after the surgery.
How long will I be on medication after the cataract surgery?
You will be on medication (application of antibiotic and steroid eyedrops) for several weeks after the surgery.
What medical instructions do I have to follow after the surgery?
- Before applying the prescribed eyedrops, wash your hands thoroughly and shake the bottle well before use.
- Tilt your head backwards and gently pull down the outer edge of the lower eyelid to apply the eyedrops. Gently squeeze the bottle – one drop is sufficient for each application.
- To prevent contamination of the bottle, avoid touching your eye and eyelashes with the bottle tip.
- Discard and use a new bottle if the bottle becomes contaminated.
- After applying the antibiotic and anti-inflammatory eyedrops, wait approximately 15 minutes before applying the lubricant eyedrops.
- Do not use the same set of medication for each eye.
How many days of medical leave for cataract surgery?
You will be given hospitalisation leave of between 1 and 4 weeks although most patients are able to resume work 1 week after the surgery.
What do I need to avoid after cataract surgery?
- Avoid prolonged reading, computer work and watching television during the first 12 hours after surgery.
- Do not drive nor operate heavy machinery during the first 24 hours.
- While sleeping, use the eye shields provided during the first week to prevent the accidental rubbing of your eyes while asleep.
- Avoid travelling during the first week.
- Stay away from dusty and smoky areas the first week to prevent particles from entering and irritating your eye. It is advisable to stay indoors but if you have to leave the house, put on protective glasses.
- Avoid water getting into the eyes when washing your face or hair during the first 2 weeks.
- Do not apply any eye makeup during the first 2 weeks.
- Do not cook during the first 2 weeks.
- Avoid swimming, hot tubs, hot yoga, jacuzzi and sauna for 1 month.
- No contact sports and heavy lifting is allowed for 1 month. Use a headband during exercising to prevent sweat from entering the eye.
How much does cataract surgery cost (in Singapore)?
You can expect to pay an average of $1,269 for cataract surgery on 1 eye in a public hospital if you are a Singapore citizen and eligible for government medical subsidies. This amount includes the operation, implant, and other fees. For more information, visit the MOH website here: https://bit.ly/2EH6yPT
The average cost of a cataract surgery at 5 private hospitals is $4,490 per eye . This figure, however, can go up to $10,000 per eye, depending on how complex your condition is, how experienced the surgeon operating on you is, the type of assessments conducted, the type of IOL implanted, and the type of medication prescribed.
For private clinics, the cost of cataract surgery is comparable with that of private hospitals. The range in the breakdown of costs for surgery performed by a senior eye surgeon are as follows:
| Service | Fee |
|---|---|
| Cataract assessment | $80 to $300 |
| Cataract surgery (1 eye) | $3,000 to $10,000 |
| Post-op medication | $100 to $300 |
| Post-op review | $80 to $200 |
Can I use Medisave and insurance for cataract surgery?
Yes, you can use Medisave and insurance for cataract surgery.
For Medisave, you can claim up $2,450 per eye from either your own, spouse’s, or children’s Medisave account.
As for insurance, most policies provide coverage for cataract surgery, the amount claimable depending on the coverage of your policy.

How do I know which eye doctor or eye centre is good?
Approach only credible and reputable eye doctors and/or eye centres when considering your options for cataract surgery. Check the credentials of the surgeon and eye centre, as well as read online reviews. In addition, you can ask your family and friends for recommendations.
Things to look out for before making your decision:
- The kind of technology and medical equipment used
- The level of service quality
- Do they listen to your needs and provide an unbiased consultation?
- How transparent is the pricing; are there hidden costs and do they try to hard-sell/upsell?
- Their track record of complications arising from surgery
All things considered, select the eye surgeon/centre you feel the most comfortable with.